By Jack Adams, Talia Beechick and Madison Hopkins
Chris Nielsen’s future looked bright. A senior in high school, he played catcher on his school’s baseball team in a Chicago suburb and was offered a full scholarship to play the sport at Michigan State University. But at age 17, after his first knee surgery, he was prescribed Percocet and Dulotin to help ease post-surgery pain.
Nielsen grew up around drugs. Both of his parents were addicted to heroin, and his father died from an overdose when Nielsen was just a few years old, he said. His uncles also used, and drugs and addicts became common fixtures in Nielsen’s childhood.
“I was physically and sexually abused when I was a kid,” he said. He went to live with his grandmother where he kept his distance from drugs until his knee surgery.
“I don’t care what anybody says, it’s freaking genetic,” Nielsen said, sitting on a couch at a Gateway Treatment Center in Chicago. “I have no kids, but I’m glad I don’t, because I ended that cycle in my family.”
Like many before him, Nielsen found his way to heroin from using prescription drugs. Now, he is 35 years old and has overdosed three times from painkillers and heroin. Nielsen is one of several recovering addicts we spoke with at a Gateway Treatment Center in Chicago.
Overdose death rates have exploded across the country during the past several years, with a boom in heroin and prescription drug use widely credited as the drivers of this lethal trend. Between 2000 and 2014, the rate of deaths from drug overdose increased by 137 percent nationally. In Illinois, the average age-adjusted rate of overdose deaths increased by nearly 66 percent, according to data from the Centers for Disease Control and Prevention (CDC).
The Chicago metropolitan area ranked first in the U.S. for emergency room visits related to heroin use.
-Illinois Consortium on Drug Policy
Data from the Illinois Department of Public Health (IDPH) shows that in 2014, more than half of all overdose deaths in Cook County involved heroin. At the same time, state funding for addiction treatment has dropped, resulting in a dramatic loss of treatment capacity, especially in rural communities.
Illinois overdose deaths by selected drug
[field name=”oddeaths”]
“Ultimately those who start heroin often had their introduction to opiates with prescription drugs,” said Sally Thoren, executive director of Gateway’s West Side location. “Whether that gets expensive or suspicious, heroin becomes a cheap alternative. That’s the progression we’re seeing.”
But Dr. Scott Cooper, president of the Illinois State Medical Society, isn’t convinced.
“It’s an alarming crisis that we’re having deaths from heroin overdose,” said Cooper. “Whether there’s a perfect link between that and narcotics, I’m not sure.”
What does Dr. Cooper think about prescription drugs and heroin?
[vimeo 156597005 w=474]
“THIS IS WHAT’S BEEN MISSING”
In 2013, a young boy found a body lying in the men’s bathroom at Savers, a thrift store in Chicago. It was Kyle Forgue, with a needle stuck in his arm. He didn’t appear to be breathing.
Forgue, suffering his second heroin overdose, was 18 years old. Paramedics arrived on the scene and administered Narcan, the brand-name for naloxone, a drug that can reverse the effects of an overdose instantly.
Click on the animation below to learn more about opiate overdoses, withdrawal symptoms, and Narcan.
[vimeo 156577182 w=474]
Forgue also found heroin at the end of a long journey of moving from drug to drug. He began drinking alcohol and smoking marijuana at age 12, and at 14 he and a friend began stealing painkillers—Norco and fentanyl—from his friend’s father. By age 15, he was shooting up heroin.
“I was already addicted to painkillers to begin with—it’s a really expensive habit,” said Forgue, now 21. “Buying 15 Narcos and doing them all at once, barely getting high off it—I found out that heroin was a lot cheaper. First time I tried it, it just felt like a big relief … like this is what’s been missing my whole life.”
Several of the residents at Gateway echoed this experience. Heroin made them feel complete, like the best possible versions of themselves, they said.
“It felt like God reached down and grabbed my heart,” said Bryant O’Malley, 21. “This is the feeling I’ve been missing my whole life.”
From there, the drug hooks its users in a cycle of dependency. O’Malley said his use of heroin “skyrocketed” after his first time. Eventually he was injecting every day, until he was charged with 11 felonies in 2014, including “car hopping” and drug possession.
“It felt like God reached down and grabbed my heart. This is the feeling I’ve been missing my whole life.”
-Bryant O’Malley, 21.
“I did a year in prison and I told myself, ‘You’re not going to do heroin anymore,’” O’Malley recounted, noting that he used other drugs, marijuana and Xanax, while in jail. “When I got out of prison, I relapsed nine days later.”
O’Malley said that he was no longer using the drug to feel high, but to avoid symptoms of withdrawal. Without heroin, he felt extremely ill, making it difficult to function and keep a job without consistently using.
“I worked for a pool company, and I would just use in the morning and use while I was at work, just to feel normal so I wasn’t sick,” O’Malley said. “Just so I could work.”
Danny Cervantes, 22, agreed. “When I had it, it was like a mom’s hug and when I didn’t, it was like my dad slapped me,” he said.
Described by Thoren as “the world’s worst flu, times 10,” Gateway residents agreed that withdrawal from heroin was almost too difficult to bear without medication, such as Suboxone or methadone, to ease the transition. Both replace the drug and help frequent users detox more comfortably.
“The withdrawals…” O’Malley’s voice trailed off, a shadow passing across his face. “You feel like you’re dying. You get cold sweats, some people throw up, you get diarrhea, you can’t sleep, and you get seizures.”
Cervantes had a friend who killed himself late last year, potentially from trying to quit heroin on his own.
“When they found him, he was just in an alley, on the stairs,” Cervantes explained. “I’m pretty sure he was withdrawing. I don’t know if he couldn’t take it or what, but he shot himself.”
All nine of the Gateway residents interviewed for this article knew at least one person, if not two or three, who had overdosed. Many of them died as a result.
A PLAN FOR CHANGE
On Sept. 2, 2015, Illinois lawmakers overturned Gov. Bruce Rauner’s veto of the Heroin Crisis Act, a law designed to address opioid abuse and addiction in the state.
Addiction treatment advocates have hailed the law, saying once it’s fully implemented, it would be a huge step in the right direction toward fixing Illinois’ perilous situation with drug addiction treatment. Some key elements of the law, House Bill 1, include:
- Every law enforcement officer and firefighter in Illinois will be required to be trained to use and have access to opioid antagonists, such as Narcan;
- Illinois’ Medicaid program will fully cover heroin addiction treatment;
- Pharmacists are allowed to dispense Narcan to prevent heroin overdoses;
- The Illinois State Board of Education must create a heroin and opioid drug-prevention program for schools; and
- Doctors and pharmacists are required to document narcotic prescriptions.
Kathleen Kane-Willis, director of the Illinois Consortium on Drug Policy at Roosevelt University, agrees that HB 1 could help reduce Illinois’ addiction and overdose epidemic.
“House Bill 1 is a really big, sweeping, omnibus legislation that addresses so many things,” she said. “I think when we get the medication-assisted treatment under Medicaid approved and we get the Naloxone over the counter, that would be very helpful.”
What does Kathleen Kane-Willis think about House Bill 1?
[vimeo 156597002 w=474]
According to Cooper, the Illinois State Medical Society supported this bill and the Prescription Monitoring Program that allows providers to track patients’ drug-related activities.
“There is no blood test for pain,” Cooper said. ”We have to take you at face value when you say you have pain. But there are red flags.”
If the patient comes back too often to refill their prescription, Cooper said there’s a chance they’re abusing the medication. The Prescription Monitoring Program mandates that the pharmacy filling a prescription must record the name, address and the drug supplied to a central database, which the doctor who prescribed those drugs can see. With that information, doctors could address issues of abuse with their patient.
How does the Prescription Monitoring Program work?
[vimeo 156597004 w=474]
OUT OF THE ALLEYS AND INTO THE FIELDS
Shelby McCall was a dancer who struggled with low self-esteem, despite growing up in what she calls an “amazing family.”
“My whole life, I’ve always felt different, like I wasn’t good enough,” she said. “When I was 15, I started hanging out with the cool kids—or so I thought. A lot of it had to do more with fitting in. It’s embarrassing for me to say right now but it’s true,” she said.
It was these “cool kids” who introduced McCall to a variety of drugs, quickly escalating to heroin. Now, she is 20 years old and is actively getting treatment for drug addiction at Gateway.
Younger addicts are becoming more and more common at Gateway treatment centers, according to Thoren.
“The population we serve is much younger than 20 years ago,” Thoren said. “We are seeing 18, 19, 20-year-old heroin addicts who come from everywhere.”
In 2015, Roosevelt University released a report based on Kane-Willis’ research, which found the Chicago metropolitan area ranked first in the U.S. for emergency room visits related to heroin use. In addition, 35 percent of those entering treatment in Chicago reported heroin use as their reason for going. Metro East Illinois heroin admissions quadrupled between 2007 and 2012, and Decatur had a six-fold increase.
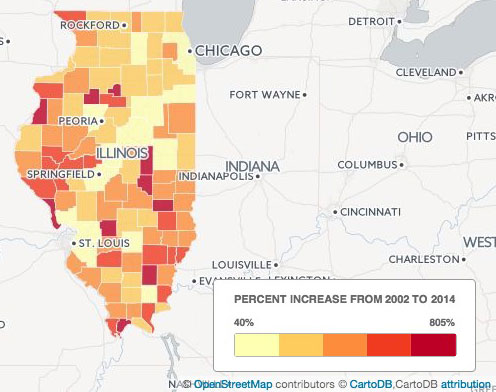
According to data from the CDC, Illinois’ rural counties have seen some of the highest increases in drug use in recent years, with some counties, including downstate Calhoun and Hamilton, seeing an 805 percent increase in the rate of drug overdose deaths between 2002 and 2014.
Some rural counties in Illinois have seen an 805 percent increase in drug overdose deaths.
-Data from the CDC
In both Pope and Hardin counties in southern, rural Illinois, the rate of overdose deaths exceeded 20 per 100,000 residents, compared to the U.S. age-adjusted rate at 14.7. Stacy Crabb, executive director of the Family Counseling Center, which serves both counties, attributes this rise to poverty in the region.
“In southern Illinois, we have pretty bad economics,” Crabb said. “So you’re obviously going to see a correlation to people using drugs.”
Saline and Gallatin counties’ rates of overdose deaths also exceeded 20 people per 100,000 residents in 2014.
Public Health Administrator Jamie Byrd of Egyptian Health Department, which serves these counties, said the community is well aware of the drug overdose epidemic.
“Our No. 1 health priority is substance abuse,” Byrd said. “Our department offers substance abuse counselors, and Suboxone treatment is available.”
LACK OF FUNDING; LACK OF OPTIONS
James McCulloch was a straight-A student who played basketball and football in high school. Once he began making friends with students who did drugs, however, he proceeded down the line from marijuana to cocaine to ecstasy to painkillers and, eventually, to heroin.
“It is hard to get treatment, it is hard to get help,” said McCulloch, 27. He went to the emergency room twice, was prescribed Xanax and was sent home without treatment.
“The window of opportunity to help someone with heroin is very small,” McCulloch continued. “When you’re out and you’re sick and you want to get help, but you call someone up and they say, ‘Well, can we call you back?’ or ‘How about the next day?’ In that second, you’re going to decide, ‘f–k it.’ You’re going to go get money and you’re going to use again.”
While heroin use is increasing, the study by Roosevelt University found that the state’s ability to treat addiction is declining.
In 2012, heroin admissions for state-funded treatment centers in Illinois were more than 56 percent higher than the national average. Meanwhile, Illinois had the largest drop out of any state in its capacity to treat addiction, losing more than half of its treatment episodes between 2007 and 2012.
This ranks Illinois as the third worst state in terms of providing publicly funded addiction treatment, ahead of only Tennessee and Texas.
Illinois is the third worst state in terms of providing publicly funded addiction treatment centers.
-Illinois Consortium on Drug Policy at Roosevelt University
According to Kane-Willis, Illinois’ state budget woes during the past few years have led to cuts in funding for treatment facilities. In fact, general revenue funding for addiction treatment dropped by nearly 30 percent since 2007 in Illinois. In the proposed budget for fiscal year 2016, there is a 61 percent decrease compared to 2013, excluding Medicaid funding. With it, it still shows a 28 percent drop.
“There’s not really anyone who lobbies on behalf of people who have substance abuse disorders, so it’s been easy to cut funding for those kinds of programs,” Kane-Willis said. “So historically it has been a problem, and then we have this budget impasse that has made it worse.”
Why is Illinois one of the worst states in the U.S. for addiction treatment funding?
[vimeo 156597001 w=474]
Even for facilities with budgets that were never officially cut, the absence of a state budget and a reliable funding source can force many smaller facilities into temporary closure, further diminishing the state’s funding capacity, she added.
“I would argue that the problem in Illinois is significant and severe, but the lack of providing treatment is much more of a problem,” Kane-Willis said. “That’s really where we’re falling down.”
“If it’s not a problem and you don’t want to fund it, then quit arresting us for it.”
-James McCulloch, 27
McCulloch is frustrated at the state’s inability to fund treatment centers while it continues to incarcerate men and women for drug possession and use.
“If it’s not a problem and you don’t want to fund it, then quit arresting us for it,” McCulloch said.
According to the National Institute on Drug Abuse (NIDA), substance abuse costs the U.S. over $600 billion annually in treatment and criminal justice costs. A report from NIDA states, “the average cost for one full year of methadone maintenance treatment is approximately $4,700 per patient, whereas one full year of imprisonment costs approximately $24,000 per person.”
The report also notes that every dollar invested in addiction treatment programs yields a return of between $4 and $7 in reduced drug-related crimes and criminal justice costs. While relapse among drug addicts can occur, NIDA’s report said it is important to not dismiss treatment as unsuccessful. Instead, relapse signifies a need for treatment to be reinstated or adjusted.
Several of the Gateway residents had been in treatment previously. Forgue has been admitted to rehab centers seven times before, while this was Shelby McCall’s fourth time in treatment in the past year.
“I’m going to overcome this,” McCall said. “I’m going to be able to use this to make myself that much more driven to do what I want to do and to prove to everyone that you can come out of this. It’s the hardest thing I’ve ever done in my entire life. I’m not giving up.”
The Gateway Foundation has alcohol and drug treatment centers in five states, servicing a total of about 10,000 clients. According to Thoren, the Illinois centers serve roughly 450 inpatient residents and more than 700 clients on an outpatient basis.
“Our method is grounded in mindfulness,” Thoren said. “We focus on the here and now, without worrying about tomorrow.”
Thoren said the goal is to start clients with the highest level of support—residential treatment—and gradually move them toward independence through outpatient programs of varying intensities. This process as a whole can take about four months.
“We help them learn to cope with stresses without getting high, we work with families, and we teach them about addiction as a disease,” Thoren added.
Treatment for addiction doesn’t relieve the growing need for emergency overdose intervention. The Chicago Recovery Alliance (CRA), an advocacy and outreach group, has distributed naloxone and clean needles to members of the community since 1996 to avoid overdose and disease transmission. Though it wasn’t legal to obtain naloxone without a doctor’s prescription until the implementation of the Heroin Crisis Act this past year, CRA founder Dan Bigg said the group has always believed that providing naloxone was good medical practice.
“It’s unrealistic to think we would have doctors running around the streets of Chicago, writing naloxone prescriptions for people who use opiates,” said John Gutenson, a CRA employee.
Gutenson was addicted to heroin, but has been clean for 20 years. While addicted, Gutenson said he overdosed several times, and was revived by doctors using naloxone.
“Keeping people alive and disease-free long enough to figure things out seems to be the logical thing to do,” said Gutenson.
Law enforcement departments in DuPage County and elsewhere have issued naloxone kits to officers to administer in overdose emergencies. For now, the Gateway residents continue to pursue recovery.
“If I don’t stay in recovery and do the things that I need to do to stay clean and sober, I’m going to die from heroin,” Shelby McCall said. “I’m just going to die someday without doing anything with my life. Because I can give away one thing, which is heroin, and have everything else in the world.”