Zika Virus: The facts, the fears and the future

By Neil Murthy A Medill Newsmakers Report The current Zika Virus epidemic first began in Brazil last year, and has since spread to more than 25 countries throughout Latin America and the Caribbean. With the World Health Organization declaring the virus to be a “public health emergency of international concern,” the CDC, along with state […]
The deal with diet pills—Weight loss supplements remain a ‘Wild West’

By Neil Murthy Meet Whitney—a 42-year-old wife and a mother living on the North Shore. Her favorite pastimes include performing in musical theater, actively participating in her child’s PTA, volunteering with various local charity organizations and mentoring her 7-year-old daughter’s busy round of school, homework and sports. She is also on a decades-long quest to […]
EPA Calls for More Oversight On Lead Following Flint Water Crisis

By Neil Murthy In the wake of the lead crisis in Flint, Mich., the U.S. Environmental Protection Agency is calling for increased oversight and collaboration with state and local water agencies to prevent additional problems with lead. On Feb. 29, the EPA wrote a letter to all state governors and state environment and public health […]
FDA gives top priority to protecting the blood supply from Zika virus

By Neil Murthy The Food and Drug Administration is turning to technology to protect the nation’s blood supply from Zika, as the virus continues to sweep across the Americas and Chicago reported the first case here last week. Currently there have been no confirmed cases of Zika virus transmission through blood transfusions in the United […]
Children explore the universe of science at Family Science Day

By Neil Murthy Children explored robotics and met a NASA astronaut as they delved into experiments at the Family Science Day hosted by the American Association for the Advancement of Science (AAAS) annual conference in Washington, D.C. AAAS is the world’s largest general science society and brings together leaders from multiple disciplines to share their […]
Inside Syria: Trapped on the frontlines of war

By Neil Murthy What is life like for the thousands of Syrians who have not left their country but are displaced at camps on the fringes of their own borders? As the Syrian civil war enters its fifth year, the devastation in the country continues to escalate a humanitarian crisis with the largest displacement of […]
From Ebola to Zika: How Lessons from Ebola Might Guide Zika Response
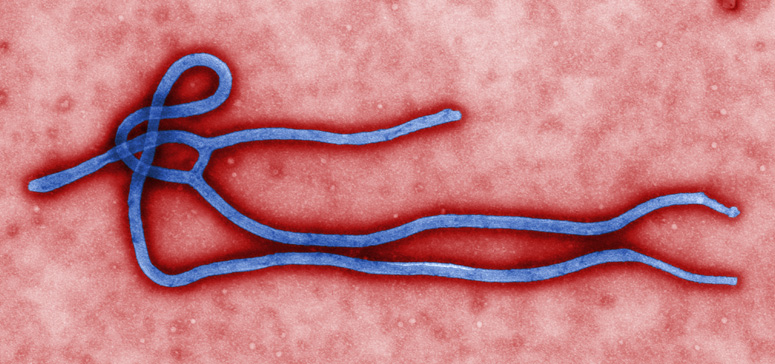
By Neil Murthy Health officials are turning to strategies learned during the Ebola pandemic to combat the burgeoning Zika virus epidemic. Dr. Ana Maria Henao-Restrepo, a medical epidemiologist from the World Health Organization, described her experience testing an experimental Ebola vaccine during the outbreak in Guinea in 2015. A Zika vaccine is still in the […]
World Health Organization calls emergency meeting on global threat of Zika virus

By Neil Murthy The World Health Organization will hold an emergency meeting Monday to consider whether Zika should be designated a global health crisis, in light of the spreading virus linked to birth defects. “We need to take action now,” said Dr. Margaret Chan, WHO’s Director-General, speaking at an informational session at the organization’s headquarters in Geneva Thursday. […]
Public health experts urge World Health Organization to ramp up Zika response
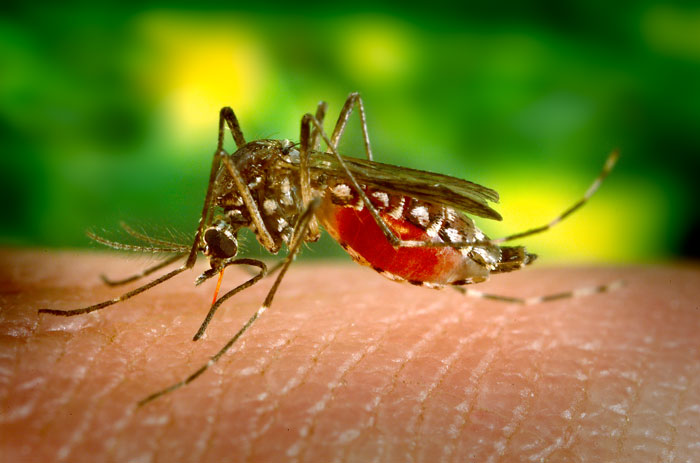
By Neil Murthy Public health experts are calling for the World Health Organization to step up efforts in the fight against the Zika virus outbreak. In the Journal for the American Medical Association viewpoint article published Wednesday, a doctor and public health lawyer urge WHO to utilize lessons learned from the Ebola epidemic and formulate […]
