By Lily Williams
[vimeo 193601521 w=474]
Tackling an abnormal protein in the brain may chart the way to holding off the onset of Alzheimer’s disease. Northwestern University’s Feinberg School of Medicine is part of a global consortium conducting clinical trials to prevent Alzheimer’s disease years before the first symptoms appear.
Dr. Borna Bonakdarpour, a neurologist at Northwestern’s CNADC, or Cognitive Neurology and Alzheimer’s Disease Center, is using brain scans as the part of the A4 trials. The trials are aimed at slowing the progression of Alzheimer’s in people who have abnormal proteins in their brains, but who do not yet have Alzheimer’s symptoms.
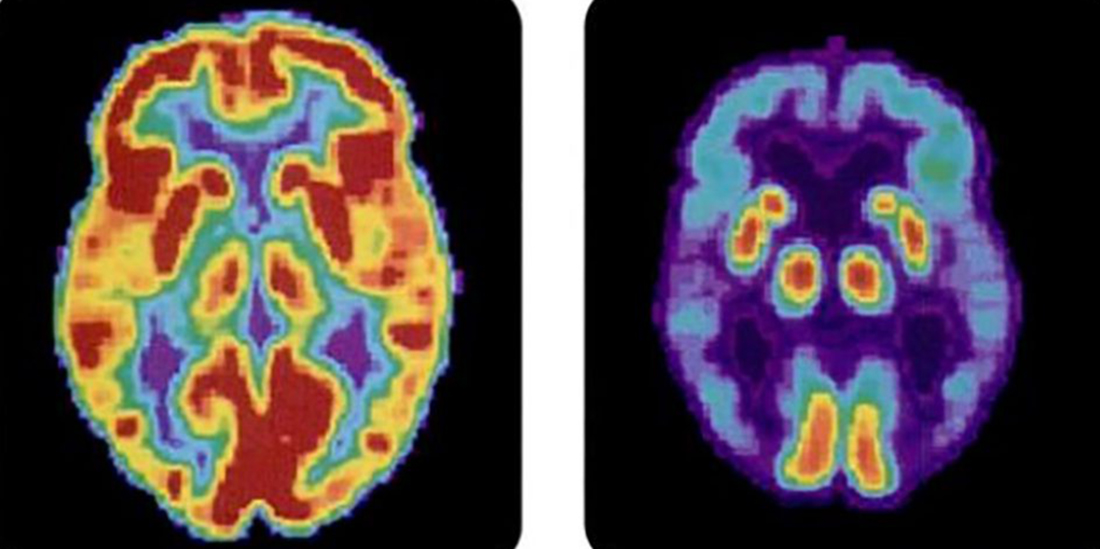
“Alzheimers pathologies start building up even 20 years before people are symptomatic,” said Bonakdarpour, an expert on changes in the brain that can impact language. “With the advances we’ve had in biomarkers and imaging we are able to find those abnormal proteins using a PET scan,” in which a person receives an injection of dye that will light up in a scanner if it hits spots with disease potential. “We can see the people with these proteins and offer them treatment.”
When Bonakdarpour says “proteins,” he is referring to two substances that, when found in the brain, are closely linked with Alzheimer’s disease. One of these substances is called amyloid plaque, and it builds up around neurons like the plaque that clogs your teeth. The other substance is called tau protein and it becomes tangled among the neurons when in contact with these plaques. These substances cluster the brain and cause decreased memory capabilities.
The A4 trials are testing a drug called solanezumab, which binds to the toxic amyloids in the brain and brings them to the periphery for excretion. Researchers’ goal with the drug is to slow the buildup of these proteins and prolong the onset of Alzheimer’s. Test patients receive either the drug or a placebo once a month via an intravenous injection.
But there is still much to learn about Alzheimer’s. The disease could also have immune or hormonal influences as well, said Bonakdarpour.
Dr. Mark W. Albers at Massachusetts General Hospital’s department of neurology, also focuses on predictive Alzheimer’s research. While he doesn’t work directly with the A4 trials, he said he knows them well.
“My sense is that, particularly in these early stages, there are many different diseases that move forward and progress and finally have one pathway that we call Alzheimer’s. In order for us to have an impact, we need to diagnose it at a molecular level,” said Albers.
The complexity of the disease necessitates these clinical trials, which use human subjects as opposed to rats or mice. The A4 trials rely on people to volunteer for the testing. Bonakdarpour said the study uses outreach, lectures and other methods to attract volunteers to the study. Finding participants is a constant process.
“One of the issues is that because people don’t have symptoms and are normal, they are less likely to come to us. But it’s very important for people to participate, as kids participated in polio vaccine, for example. They just volunteered. They didn’t have these diseases, and that’s how we found out those vaccines worked,” he said.
If Bonakdarpour’s scans show abnormal proteins, volunteers over 65 will enter the experiment for three years. Recruitment for the trials is still going on, and with the three-year experiment and a year of data analysis, it could be until 2020 before the experiment is finished. Other trials may approve solanezumab for the market before the A4 trials are done, but only for symptomatic patients.
Researchers are working on a number of other Alzheimer’s clinical trials. Bonakdarpour is testing another path with Suzanne Craft, a Ph.D. gerontologist at Wake Forest University. They are studying what they call a “type III diabetes,” where the brain does not have enough insulin for sugar uptake, causing memory loss. The researchers delivered insulin to the hippocampus (the brain’s memory center). In a study of 100 patients, this insulin delivery demonstrated slower Alzheimer’s progression. Bonakdarpour and Craft are currently moving into the next phase of the trial with a larger number of participants.
However, a crucial, but often forgotten aspect of all of these preventative studies is the ethical questions they pose. “They [researchers] will tell people whether they are amyloid positive or not, and they’re doing research on how to do that ethically. Even if the trial fails, they are going to learn about how to deal with this charged issue. It can cause a lot of concern and worry and have a negative impact on people’s quality of life.” said Albers.
Studies of Alzheimer’s may be more important than ever, as over 15 million baby boomers are predicted to get Alzheimer’s, according to Kevin Connolly, an administrator at the center. Federal funding for Alzheimer’s is also increasing, where funding for other diseases remains flat, said Connolly. Soon, funding could be up to $1.4 billion.
“It would be fantastic if we get help from a lot of people who are interested in finding a solution for this horrible disease,” said Bonakdarpour.